
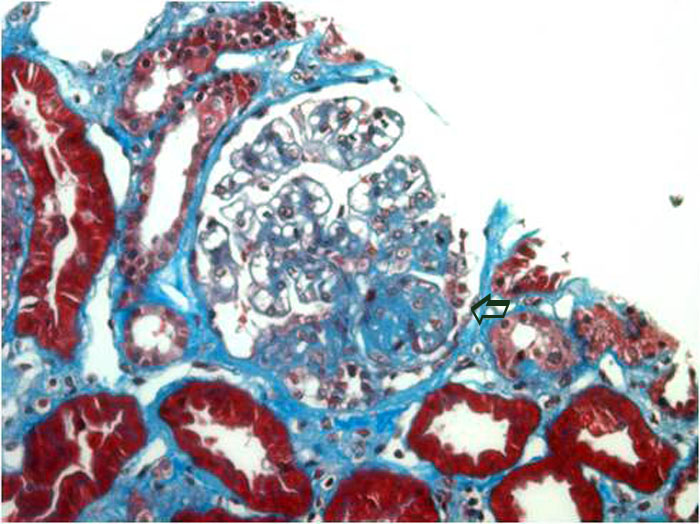
Trichrome shows nodular sclerosis concentrated at the glomerular hilus. The rest of the glomerulus appears normal. Note the lesion is "focal" in that the areas apart from the sclerosis appear normal. There is a suggestion of mild fibrosis in the intersitium.
PAS stain shows another sclerotic lesion at the hilar region. Adhesion (also called synechia) of the sclerotic tuft to Bowman's capsule is common. Note the striking hyalinosis.
Focal segmental glomerulosclerosis (FSGS) is so named because sclerosis affects some but not all glomeruli (focal), and in the affected glomeruli, only a portion of the tuft is involved (segmental). These lesions are first seen in the corticomedullary junction and spreads outward toward the periphery, thus, if the biopsy is not deep enough, this diagnosis may be missed. The underlying pathology of FSGS, is related to injury of the foot processes of the podocytes. Thus, FSGS is included in the category of "podocytopathies".
Major morphologic distinctions exist between the three major categories of FSGS.
(1) The "classic" form of FSGS demonstrates perihilar sclerosis, where the lesion arises adjacent to the afferent arteriole.
(2) In "glomerular tip lesion", the sclerosis occurs at the tip of the glomerular tuft or where the proximal tubule originates. This variant supposedly connotes an improved prognosis, although this assertion is controversial.
(3) In the collapsing glomerulopathy variant, there is a segmental or even global collapse of the glomerular tuft leading to obliteration of capillary lumina. This form is strongly associated with HIV and IV drug abuse. This variant has a particularly rapid course and poor prognosis.
This case will refer to the classic (perihilar) form of FSGS, where the segmental sclerosis is seen in the perihilar region of the glomerulus. The sclerotic segment often seems adhered to Bowman's space. Early lesions may demonstrate hypercellularity of the mesangium and as the disease progresses, sclerosis occurs and the lesions becomes hypocellular. Hyalinosis, which is the result of insudation of protein between endothelial cells and the glomerular basement membrane, is also a feature.
On immunofluorescence, there is nonspecific staining pattern of IgM and C3 in the sclerotic tuft, which represents entrapment of these entities and not immune-mediated disease (Zhou).
FSGS can be further subdivided into idiopathic (primary) or secondary causes. The diagnosis of idiopathic FSGS can only be made after secondary causes have been ruled out.
Secondary FSGS largely arise from the loss of renal tissue -- leading to hyperfiltration of the overburdened remaining nephrons. This loss of renal parenchyma can result from long-standing hypertension, obesity or single kidney -- furthermore, enlarged glomeruli (glomerulomegaly) may be seen as another compensatory change.
Frequently a cause of nephrotic syndrome and in adults. It is the predominant cause of nephrotic syndrome in African Americans. In some studies, FSGS surpasses even membranous nephropathy or IgA nephropathy as the most common cause of nephrotic syndrome in adults (Kumar, Zhou).
A good prognostic feature of primary nephrotic FSGS is if it responds to corticosteroids. Alkylating agents are mostly ineffective in the steroid-resistant forms. Corticosteroids and cyclosporine A remain the mainstay of treatment.
40-60% of patients develop end stage renal disease within 10 to 20 years, and of those that undergo renal transplantation, recurrence in the tranplanted kidney is seen in 15 to 50% percent of patients (Rosai). Tubulointerstitial damage, as demonstrated by interstitial fibrosis and tubular atrophy, is useful as an indicator of disease progression (Rosai).
• Kidney : Focal Segmental Glomerulosclerosis, Collapsing Glomerulopathy
• Kidney : Focal Segmental Glomerulosclerosis, Glomerular tip lesion
Jeannette JC, University of NC at Chapel Hill. Renal Pathology Tutorial. Last viewed on 7 November 2010. Available at: www.uncnephropathology.org/jennette/tutorial.htm
Kumar V, Abbas AK, Fausto N. Robbins and Cotran Pathologic Basis of Disease. 7th Ed. Philadelphia, PA: Elsevier; 2005: 962-4.
Rosai, J. Rosai and Ackerman's Surgical Pathology. 9th Ed. Philadelphia, PA: Elsevier; 2004: 1171-3.
Zhou M, Magi-Galluzzi, C. Genitourinary Pathology: Foundations in Diagnostic Pathology. Philadelphia, PA: Elvesier; 2006: 354-8.
Dr. Jeannette has a very nice tutorial online regarding FSGS referenced above. Particularly, his categorization of FSGS is simple and easy to understand, which is depicted in this image: www.uncnephropathology.org/jennette/fsgs/tut24.jpg