
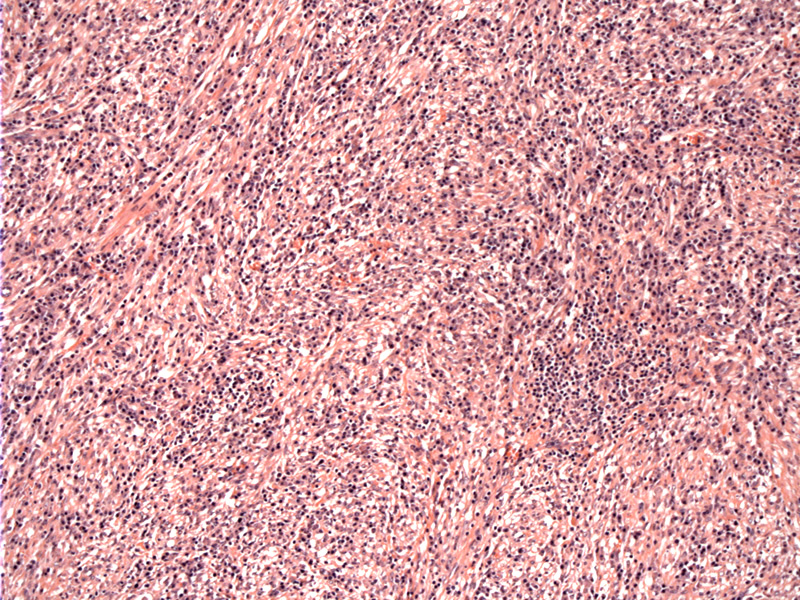
A compact proliferation of spindle cells are admixed with many chronic inflammatory cells.
Lymphocytes and numerous plasma cells are evident, a key feature in inflammatory myofibroblastic tumors.
Inflammatory myofibroblastic tumor most commonly occurs in the lung but may be seen in a variety of extrapulmonary locations. Coffin et al (1995) reviewed 84 extrapulmonary IMTs and found that 61 cases occurred in the pelvis, 12 cases in the head and neck, 8 cases in the trunk and 3 cases in the extremities.
Most extrapulmonary IMTs arise in children (average age of 9) and can present with constitutional symptoms (fever, weight loss, pain) and laboratory abnormalities (anemia, thrombocytosis, polyclonal hypergammaglobulinemia, elevated ESR)(Coffin).
IMT is a nonmetastasizing proliferation of myofibroblasts and rarely behave in a malignant fashion (Fletcher). Morbidity and mortality may result from local obstructive growth and treatment-related complications (Coffin).
• Spleen : Inflammatory Pseudotumor
• Bladder : Urachal Inflammatory Myofibroblastic Tumor
• Liver : Inflammatory Myofibroblastic Tumor
• Lung : Inflammatory Myofibroblastic Tumor
Coffin CM, Watterson J, Priest JR, Dehner LP. Extrapulmonary inflammatory myofibroblastic tumor (inflammatory pseudotumor). A clinicopathologic and immunohistochemical study of 84 cases. Am J Surg Pathol. 1995 Aug;19(8):859-72.
Fletcher CDM, ed. Diagnostic Histopathology of Tumors. 3rd Ed. Philadelphia, PA: Elsevier; 2007: 891.